
This type of curve pattern was not seen in the previous study of Buhr and Cooke from 1959 suggesting that these fractures are on the rise. Interestingly, the distribution of distal humerus fractures showed a ‘unimodal older woman’ pattern and falls in what they describe as an osteoporotic curve pattern. They reported an incidence of distal humeral fractures of 5.8 per 100,000 and noted that this was only 0.5% of all fractures seen. Court-Brown and Caesar reported on the development of fracture patterns in a stable population of around 500,000 people around Edinburgh. With an increasingly aging population in most countries in the western world, it is of value to know the likely outcome of fracture fixation of the distal humerus in this age group. Level of evidenceĭistal humeral fractures in the elderly population are on the rise and only little literature exists regarding the fixation. 
Although the rate of complications is higher than in younger patients, complications such as non-union are often asymptomatic, patient satisfaction scores are high, and the possible devastating complications of failed elbow replacement can be evaded. Advanced age should not be seen as a contraindication for ORIF of fractures of the distal humerus. The present data support indication for open reduction internal fixation (ORIF) even in the elderly patient. Our results regarding the surgical approach showed significantly higher patient satisfaction scores in the osteotomy group, compared to the group with Triceps-On Approach (PTOA). There were no infections in the presented cohort. 7 patients had radiological evidence of at least partial non-union with one requiring revision, 2 discrete hardware dislocations were treated conservatively. 6 patients developed heterotopic ossification without significant effect on the clinical outcome. Average Mayo Elbow Performance (MEPS) score was 88.7 (min. Average pronation and supination was 68.3° (min. 150° SD ± 16.5) and average loss of extension of 20.9° (min. 9 years, SD ± 2), the average range of motion was flexion of 127° (min. ResultsĪfter a mean follow-up period of 3.8 years (min. Primary outcome measures were Mayo Elbow Performance Score, VAS and joint range of motion, secondary was radiological evaluation. Patients were evaluated based on clinical criteria. 
22 patients were treated with double plate, 4 with single plate, and 1 with screw fixation only. All patients underwent the identical aftertreatment protocol with no weight bearing for 6 weeks and weekly increasing range of motion. Methodsīetween 20, 30 patients with a mean age of 78 years at the time of injury with a recent distal humerus fracture were evaluated. We hypothesized that despite advanced age, reasonable clinical results can be achieved, using a standardized surgical technique and aftertreatment protocol for the treatment of distal humerus fractures in elderly patients. The purpose of the present study was to investigate the clinical outcomes after open reduction and internal fixation and to evaluate whether the results justify reconstruction even in elderly patients. 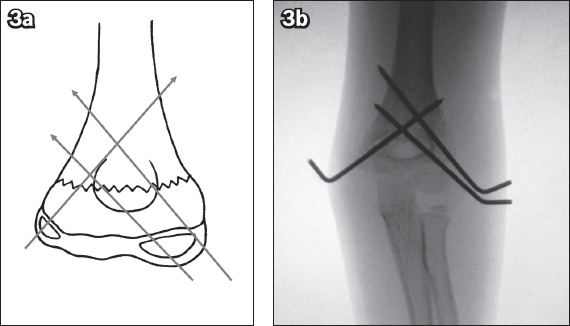
However, because of a high rate of complications related to total elbow prostheses, reconstruction of distal humerus fractures should still be considered a therapeutic option, also in the elderly patient. Due to the complexity of distal humerusfractures and often poor bone quality in elderly patients, these entities remain a challenge.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
